Wisdom tooth extraction
Wisdom teeth do not always need to be removed. Some can function normally for years, but when there is not enough space, the tooth is malpositioned, or it erupts only partially, it can become a source of inflammation, pain, and damage to the adjacent tooth. In such cases, extraction is not “prevention” but treatment.
Before making a decision, the clinical situation is assessed: whether there is inflammation, how the roots are positioned, how close the tooth is to the nerve, and whether it can be cleaned properly. This determines the extent of the procedure — from a simple extraction to a more complex surgical procedure.
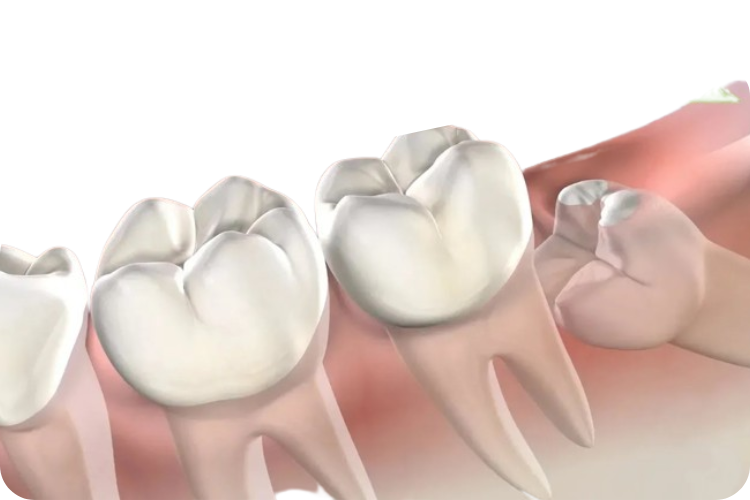
When a wisdom tooth needs to be removed
Pericoronitis (inflammation around the tooth)
Incorrect position in the bone
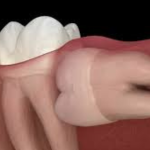
Damage to the adjacent tooth
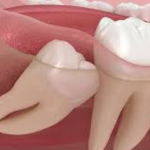
Orthodontic indications
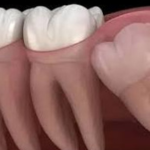
Simple and complex wisdom tooth extraction
The complexity is determined not by the size of the wisdom tooth, but by its position in the bone, the direction of growth, the shape of the roots, and its proximity to anatomical structures (the inferior alveolar nerve and the maxillary sinuses). Before the procedure, these factors are assessed clinically and on an X-ray or CT scan, which helps predict the scope of the surgery.
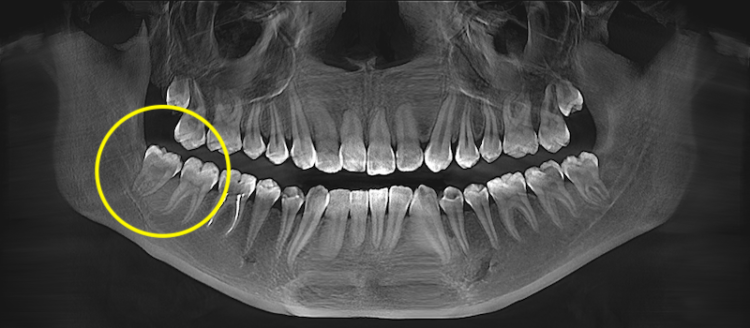
Simple wisdom tooth extraction
The wisdom tooth has fully erupted, is accessible to the instruments, the bone does not cover the crown, and the roots have typical anatomy. In this case, there is no need for a gum incision or removal of bone tissue.
After anesthesia, the tooth is carefully removed from the socket. If needed, a hemostatic sponge is placed in the socket to control bleeding and stabilize the clot. Sutures are usually not required, and recovery is faster.
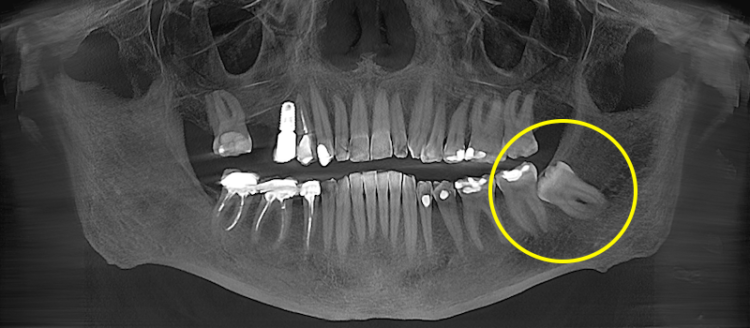
Complex wisdom tooth extraction
The wisdom tooth is partially or fully located in the bone (impacted) or has an abnormal eruption path (malpositioned). The crown may be covered by bone, and the roots may be close to the nerve or have a complex shape.
For controlled access, a gum incision is made and, in some cases, part of the bone is removed. The tooth may be sectioned into fragments, after which a hemostatic material is placed in the socket and sutures are applied. Recovery takes longer.
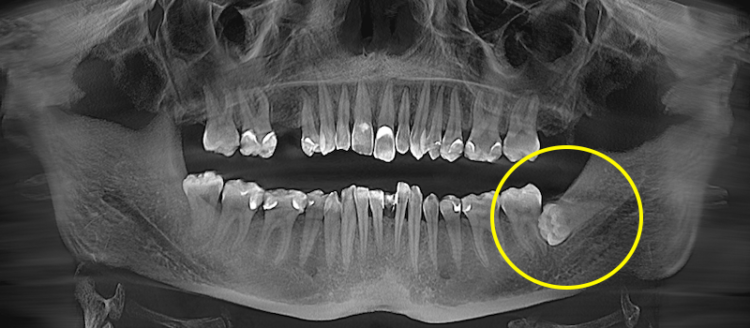
Impacted wisdom tooth extraction
An impacted wisdom tooth is a tooth that has not fully or partially erupted and remains in the bone or under the gum. Such a tooth may not cause symptoms for a long time, but it can create a risk of inflammation, damage to the adjacent molar, or cyst formation.
Before extraction, its position must be assessed on an X-ray or CT scan: the depth of impaction, angulation, root shape, and contact with the inferior alveolar nerve. This makes it possible to plan the surgical access and minimize risks.
During the procedure, surgical access to the tooth is created; if necessary, part of the bone is removed or the tooth is sectioned into fragments for controlled removal. After extraction, the socket is cleaned, irrigated, a hemostatic sponge is placed, and sutures are applied.
Recovery usually takes longer than after a simple extraction and may be accompanied by swelling or limited mouth opening in the first few days.
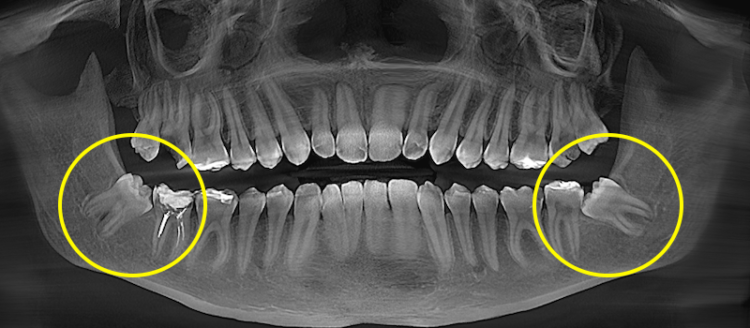
Malpositioned wisdom tooth extraction
A malpositioned wisdom tooth is a tooth that has erupted or partially erupted but occupies an incorrect position in the dental arch. Most often, it is tilted toward the second molar, grows at an angle, or is displaced toward the cheek or the tongue.
Before extraction, its position is assessed on an X-ray or CT scan: the direction of angulation, root shape, contact with the adjacent molar, and the condition of the bone tissue. This helps determine whether there is a risk of damage to the second molar and choose the optimal extraction technique.
During the procedure, the doctor carefully removes the tooth from the socket. If the tooth has a pronounced tilt or a complex root anatomy, it may be sectioned into fragments for controlled removal without excessive pressure on the bone.
After extraction, the socket is cleaned of tissue remnants, rinsed with an antiseptic solution, and a hemostatic material is placed if needed. Recovery is usually accompanied by mild swelling or discomfort in the first few days.
Cost of wisdom tooth extraction
Simple wisdom tooth extraction
from 2,900 UAH
Surgical wisdom tooth extraction
7,400 UAH
Injection anesthesia
500 UAH
Hemostatic sponge
800 UAH
Socket suturing
800 UAH
Payment
We do not have any hidden fees. Payment is made according to the price list and the agreed treatment plan.
You can pay in cash or by card (via a bank terminal).
Treatment can also be provided through an insurance claim via an insurance company or under a contract with another organization.
Clinic locations in Kyiv
The most convenient way to reach our dental clinics is from the following districts of Kyiv:
To the clinic at: Kyiv, 25B Novomostytska St. — Vynohradar, Kurenivka, Obolon, Syrets, Minskyi Masyv.
To the clinic at: Kyiv, 20 Pidvysotskoho St. — Pechersk district, Zvirynetska metro station.
To the clinic at: Kyiv, 60/1 Yalynkova St. — Kharkivskyi Masyv, Boryspilska metro station, Chervonyi Khutir, Vyrlytsia, Kharkivska.
Stages of wisdom tooth extraction
Wisdom tooth extraction usually includes 5 main stages. The exact scope of the procedure depends on the position of the tooth, the anatomy of the roots, and its proximity to the nerve, but the overall sequence of the procedure is as follows.

CT scan and surgical planning
Before extraction, we perform a CT scan using Dentsply Sirona scanners. A CT scan allows us to assess the position of the tooth in the bone, the shape of the roots, their proximity to the inferior alveolar nerve, and to plan a safe approach.

Tooth extraction
If the tooth is partially or fully located in the bone, a gum incision or sectioning the tooth into fragments may be required. In complex cases, an ultrasonic piezotome is used, which allows more delicate work with the bone.

Socket cleaning
After the tooth is removed, the socket is cleaned of tissue remnants and granulation tissue. This is an important stage that reduces the risk of inflammation and helps a stable blood clot form. Proper socket management creates the conditions for normal tissue healing.

Socket treatment and suturing
The socket is rinsed with an antiseptic solution, after which a hemostatic sponge is placed if needed. This helps stabilize the blood clot and protect the wound. In complex extractions, the gum edges are approximated and sutures are applied.

Healing follow-up
After the procedure, a follow-up examination is performed to assess the condition of the socket and the healing process. The first check-up usually takes place around day 3. If sutures were placed, they are removed during a follow-up visit around days 10–12.
Tooth extraction under general anesthesia
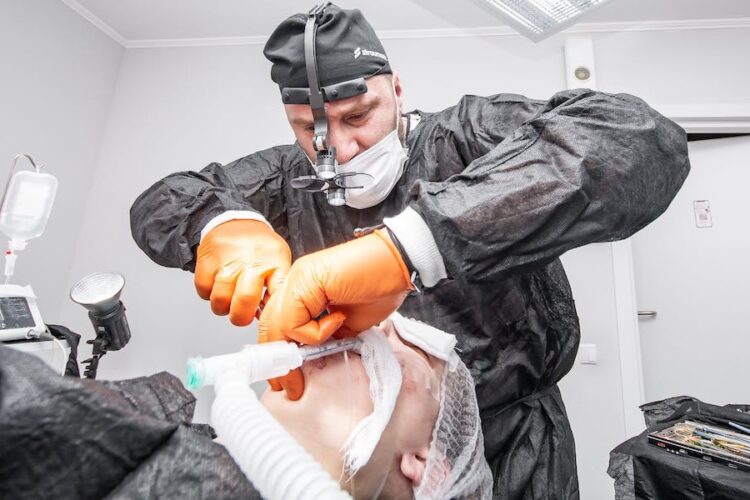
Tooth extraction under general anesthesia
General anesthesia is a controlled medication-induced sleep that the patient enters through the administration of an intravenous anesthetic with mechanical ventilation.
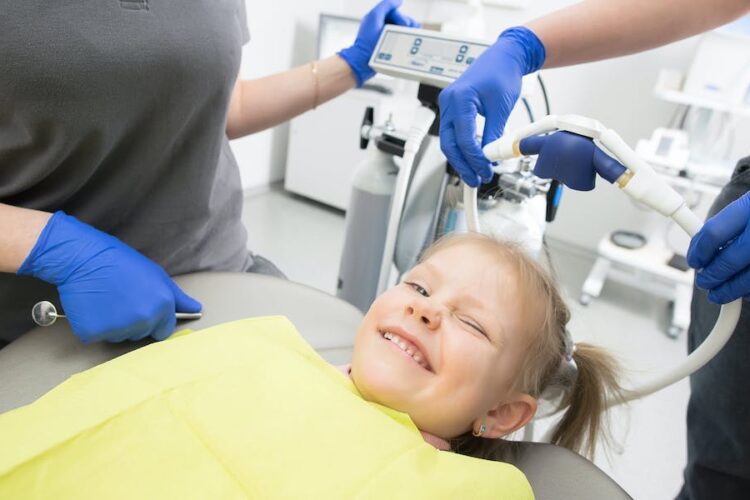
Tooth extraction under sedation
This method helps the patient relax and enter a state of relaxation and drowsiness while remaining conscious, after which the doctor additionally numbs the tooth locally.
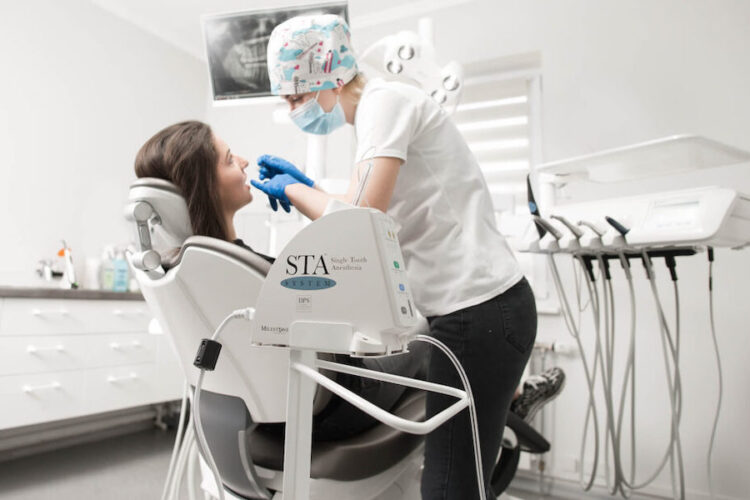
Tooth extraction under local anesthesia
The anesthetic blocks the transmission of pain impulses to the brain. As a result, for a certain period of time, the brain does not perceive pain in the area where the anesthetic works.
Recovery after wisdom tooth extraction
First 24 hours
Days 2–3
Days 4–7
Weeks 2–3
Possible complications
Swelling and pain
Moderate swelling appears within the first 12–24 hours and reaches its peak on the third day. This is a normal inflammatory response of the tissues to the procedure. Pain is controlled with pain relievers and gradually decreases from days 3–4.
If the swelling continues to increase after the third day or the pain suddenly becomes stronger instead of decreasing, this is a reason for an examination.
Bleeding
A slight oozing of blood is possible for several hours after the procedure. The blood clot in the socket is important for healing, so preserving it is essential.
Prolonged active bleeding that does not decrease after pressing a sterile gauze pad for 20–30 minutes requires a repeat examination.
Dry socket (alveolar osteitis)
Occurs in about 2–5% of cases, more often after extraction of lower impacted teeth. The cause is the destruction or absence of the blood clot that protects the socket and ensures normal tissue healing.
It presents as intense pain on days 3–5 after extraction, which may radiate to the ear or temple, bad breath, and a feeling of an “empty” socket. It requires local treatment, socket cleaning, and placement of a medicated dressing in the clinic.
Limited mouth opening
After complex extraction of lower teeth, a reflex spasm of the chewing muscles is possible. The patient may find it difficult to open the mouth widely for 2–4 days. This is related to the reaction of the muscles and tissues to the surgical procedure in the lower jaw area.
The condition usually resolves gradually without additional treatment as the swelling decreases. If the limitation in mouth opening does not lessen over several days or is accompanied by increasing pain, a follow-up examination by the doctor is needed.
Frequently asked questions about wisdom tooth extraction
Can two wisdom teeth be removed at the same time?
Yes, if the clinical situation allows it and the patient is ready for that extent of treatment. Most often, two teeth on the same side are removed — this does not make chewing more difficult during recovery.
For complex impacted teeth or at the patient’s request, removal under sedation or general anesthesia is possible.
What happens if a wisdom tooth is not removed?
If the tooth is positioned incorrectly or is only partially erupted, it may cause chronic gum inflammation (pericoronitis), damage to the adjacent second molar, or cyst formation.
Sometimes there are no symptoms for a long time, but the pathology develops gradually. The decision is made not “just in case,” but based on clinical indications after diagnosis.
How do I know whether a wisdom tooth needs to be removed?
Indications include recurrent inflammation, pain, pressure on the adjacent tooth, decay that cannot be properly treated, or a risk of bone damage. X-ray or CT imaging plays a key role — this is what shows the position of the roots and their proximity to the nerve.
If the tooth has fully erupted and is not causing problems, removal is not mandatory.
How do I know a wisdom tooth is erupting?
Local pain appears in the back part of the jaw, along with gum swelling or a feeling of pressure. There may also be discomfort when swallowing or opening the mouth.
If a gum “hood” forms over the tooth and inflammation develops, an examination is needed.
How many days does pain last after wisdom tooth extraction?
Moderate pain usually lasts 1–3 days and gradually decreases. Swelling and discomfort typically peak on the third day.
If the pain becomes stronger on days 3–5 instead of decreasing, this may indicate a dry socket and requires an examination.
How long does wisdom tooth extraction take?
Simple extraction of a fully erupted tooth usually takes about 10–20 minutes.
Complex or surgical extraction may take 30–60 minutes, depending on the anatomy. Preparation time for sedation or general anesthesia is additional.
What is surgical tooth extraction?
Surgical (complex) wisdom tooth extraction is performed when the tooth is fully or partially located in the bone, has an unusual position, or is in close contact with the nerve.
In such cases, a gum incision is made, and sometimes part of the bone is removed or the tooth is sectioned into fragments. Sutures are placed after the procedure.
What anesthesia is used for wisdom tooth extraction?
Local anesthesia is used as standard — the patient does not feel pain during the procedure.
For lower teeth, a nerve block is used to numb the nerve in the jaw area.
Sedation or general anesthesia may also be used when indicated — for example, in cases of severe anxiety, complex procedures, or removal of several teeth at once.